Doctors Are Failing Their Gay Patients
Many physicians either missed the class that dealt with sexual health questions, or their lack of attention to the subject is a conscious choice.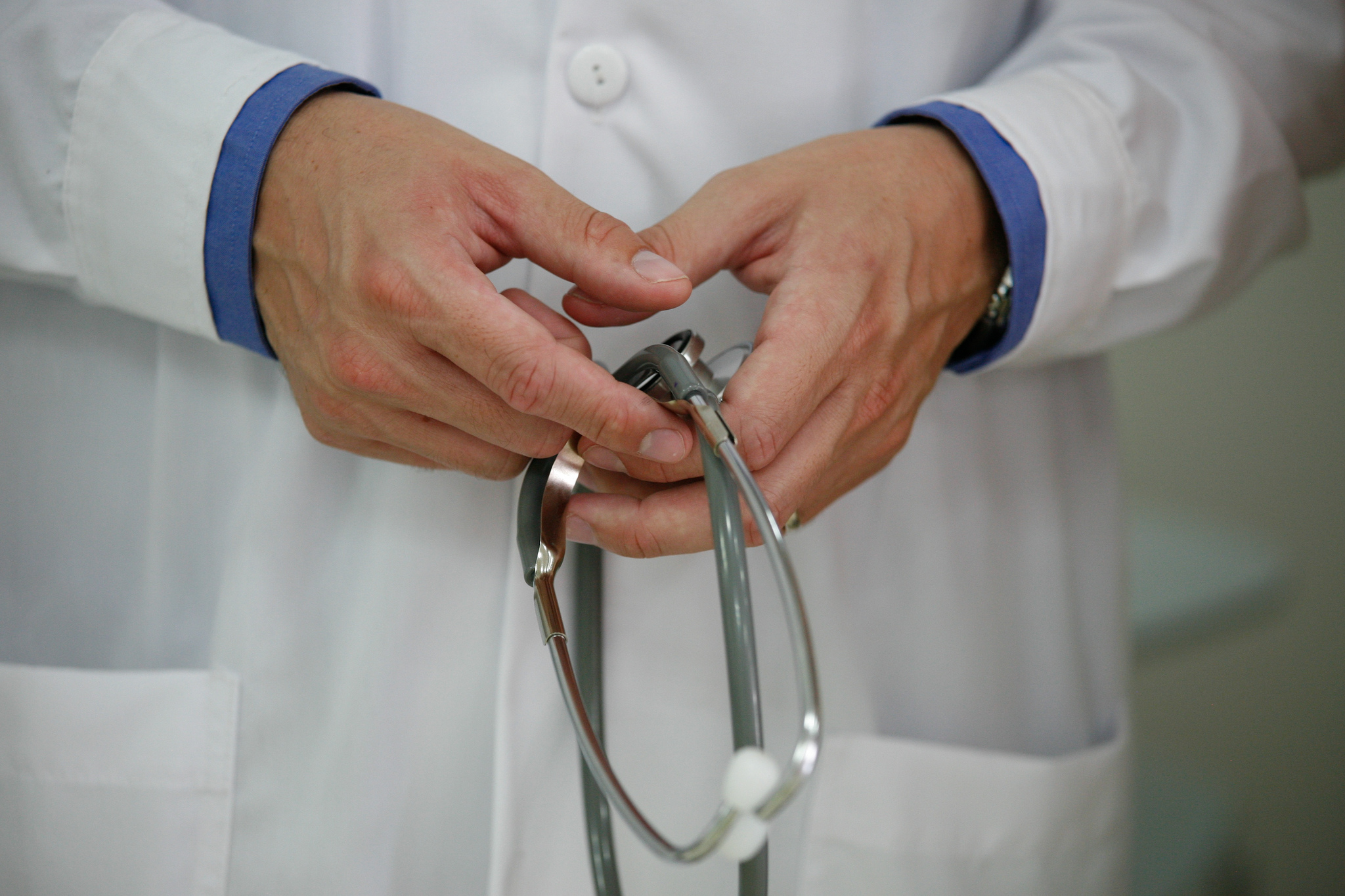 Alex Proimos / CC BY-NC 2.0
Alex Proimos / CC BY-NC 2.0
You’re supposed to be able to tell your doctor anything. But how are patients supposed to know what to tell their doctors if the doctors don’t ask the necessary questions in the first place? When it comes to sexual health screening, many doctors either missed the class in medical school that was supposed to teach them to ask patients about sexual health questions, or their lack of attention to sexual health is a conscious choice. Bespoke Surgical recently conducted a study of 1,000 Americans of various ages and sexual identities to hear what they’ve been asked by their doctor on the topic. The results suggest few doctors are asking questions about sexual health at all, and that LGBTQ patients, in particular, are being neglected.
The survey asked participants what kinds of questions their primary care physician focused on when they brought up sexual health during physical exams. The results varied based on the sexual orientation of the patient, as the graph below shows.
There are some outliers here that should be noted, but first, take a second to note how low these numbers are overall. Over half of heterosexual respondents said they were never asked about basic sexual health questions like HPV and STD exposure—a number that’s surprising, especially since 79 million Americans have HPV, a condition that can lead to cancer in both men and women. In general, it seems like doctors aren’t asking patients the right questions about sexual health.
But consider the shocking numbers revealed in the chart above. Of the physicians who saw homosexual patients last year, only 13 percent asked their patients if they had received the PrEP HIV prevention drug. Nearly half of all gay and lesbian respondents said their doctor had not asked them about HPV/Gardasil, anal pap smears, PreP/Truvada, or prior STD exposure. Only 40 percent of patients gay, straight and bi said they were asked if they used any kind of protection during sex.
When they do ask the right questions, the survey suggests doctors are asking them of the wrong people. In all but one of the above sexual health categories, bisexual patients were more likely to be asked about sexual health conditions. This could be because, as the Advocate explains, there’s a myth that bisexual people are more promiscuous than other people. The survey authors affirm this: “the ‘B’ in LGBTQ+ is often misrepresented in a variety of settings, including sexual promiscuity.”
Undoubtedly, doctors aren’t asking their patients a full range of questions because they aren’t able to spend enough time with them in the first place. People of all sexual orientations have experienced the rotating door model of doctor visits. Some primary care doctors say they treat 19 patients a day. With a full roster of 2,500 patients total, the Annals of Family Medicine says each doctor would have to “spend 21.7 hours per day to provide all recommended acute, chronic and preventive care” for that many patients. A 2016 study found that most doctor’s office visits only last 13-16 minutes. Professor Bruce Y. Lee at Johns Hopkins calls the average crammed doctor’s visit “archaic” in an article for Forbes, and says, “there is little time to actually listen or talk to patients and maybe not enough time to carefully examine them.”
The LGBTQ population seems to be catching on to the fact that primary care physicians may not know the right questions to ask their patients. That would explain why gay, lesbian and bisexual respondents were 20-30 percent more likely than straight respondents to rate having a doctor with the same sexual identity as them as “very important.” LGBTQ people are especially vulnerable to discrimination and may face barriers to health care that heterosexual people don’t. Some technology, like the entrepreneurs who launched an app to connect LGBTQ patients to gay-friendly doctors, is helping to make this easier. But it’s a quick fix to a much more systemic problem, considering so many primary care physicians don’t ask about sexual health problems at all.
Your support matters…Independent journalism is under threat and overshadowed by heavily funded mainstream media.
You can help level the playing field. Become a member.
Your tax-deductible contribution keeps us digging beneath the headlines to give you thought-provoking, investigative reporting and analysis that unearths what's really happening- without compromise.
Give today to support our courageous, independent journalists.







You need to be a supporter to comment.
There are currently no responses to this article.
Be the first to respond.