Dr. Pfau’s Leprosy Miracle
Pfau, who died last month, paved the way for humane treatment of Pakistani leprosy patients, with an approach that dramatically lowered incidence of the disease.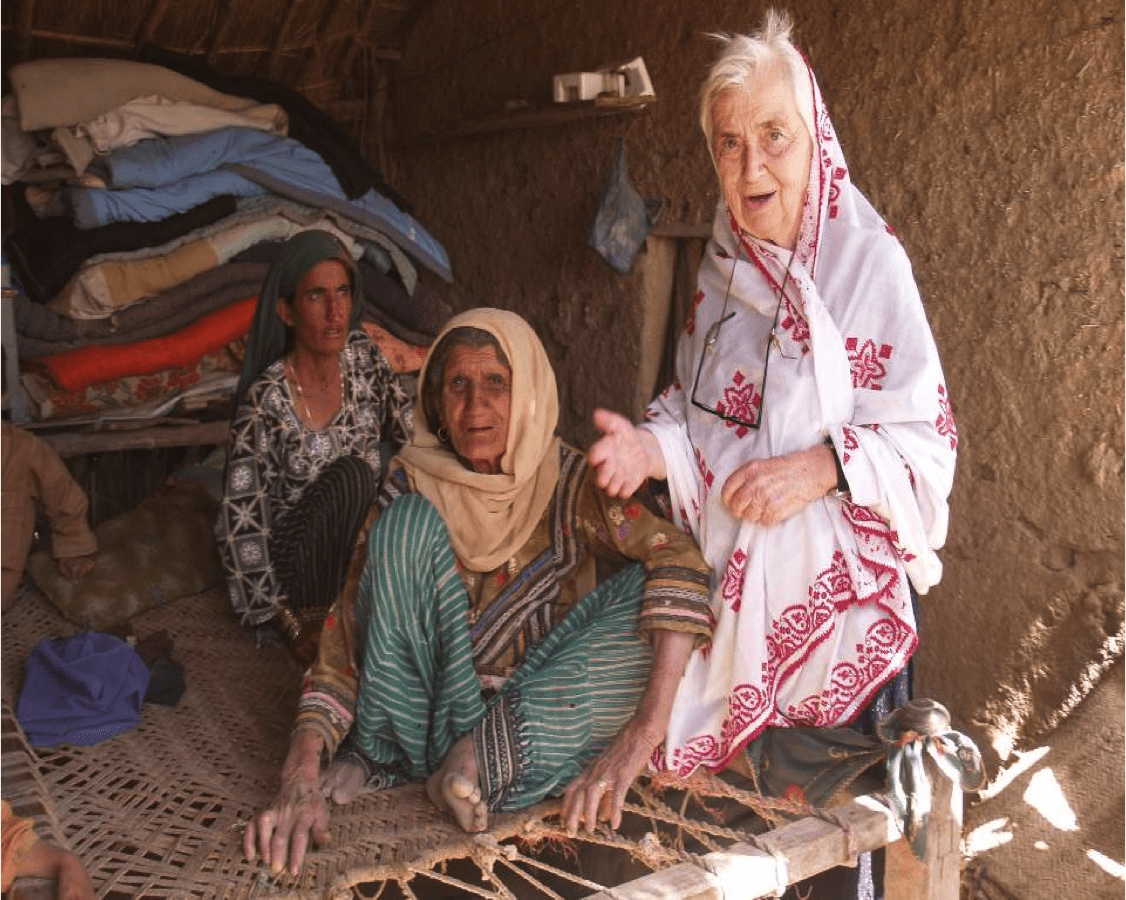 Dr. Ruth Pfau, right, with patients in Pakistan. (Marie Adelaide Leprosy Centre)
Dr. Ruth Pfau, right, with patients in Pakistan. (Marie Adelaide Leprosy Centre)
Haleema Khan (a name used in this story to preserve her anonymity) is a health management expert who is head of the secretariat in a prestigious hospital in Karachi, Pakistan’s biggest city. Efficient, professional and confident, one would never guess that Khan reached the heights of success by starting from the lowest rung of the ladder.
Khan grew up in a shanty town in the backwaters of Karachi, where she was born to parents who suffered from leprosy. This concentration of humble dwellings was home to the outcasts of society, and Khan, who had never contracted the disease herself, inherited a lowly status by virtue of her parentage. The stigma attached to leprosy has haunted her all her life (and is why she was reluctant to reveal her identity for this story).
Khan’s father developed leprosy, regarded by some as God’s curse on sinners, in 1947, when the whole of South Asia was gripped by political upheaval that led to the mass migration of 15 million people across the borders of the newly created states of India and Pakistan. Rejected by his family, Khan’s father moved to Karachi and found his way to what was derogatively called the “Lepers’ Colony.” His disease was so advanced that his hands were disfigured. Khan’s mother, who was less deformed but equally isolated, also ended up in the colony, where the residents lived like a huge family. The elders did a lot of matchmaking, and Khan’s parents ultimately tied the knot.
But the future held no hope. Christian missionaries provided medical care to ease patients’ physical sufferings, but there was no healing the scars on their souls.
Then, in 1960, a German doctor who was waiting for a visa to India, arrived at the “Colony.” She never ended up getting her visa—nor was it needed. Because within a short period of time, Dr. Ruth Pfau, a much-celebrated and widely decorated physician, Christian nun and social worker, decided to dedicate herself to the care of leprosy patients in Pakistan.
Last month, hundreds of Pakistanis—most of them Muslims—gathered at St. Patrick’s Cathedral in Karachi to pay homage and bid farewell to this remarkable woman, who died Aug. 10 at the age of 88. Pfau was given a state funeral—a rare event in Pakistan—that Pakistan’s president and other dignitaries attended.
What endeared Pfau to a people so different from her culturally, ethnically and spiritually? Her phenomenal achievement in turning leprosy into a controlled disease in Pakistan, as designated by the World Health Organization in 1996. What does this look like in numerical terms? In the 1980s, 19,398 patients were being treated for leprosy in Pakistan—a number that had dropped to 531 by 2016.
This feat wasn’t easy: It required an effective, inventive strategy on Pfau’s part.
Pfau’s miracle would never have been possible had she adopted conventional methods used by physicians and surgeons who work within the formal health system—a system that has been defined by the corporate world and mainly led by pharmaceutical giants. Money is the guiding principle in traditional health care. This holds true in all countries, developed and underdeveloped.
This explains why the Hippocratic Oath—the medical profession’s ethical code—no longer holds the sanctity it once did. By defying the corporate mindset, Pfau became a “human being who defined humanity,” as Dr. Adibul Hasan Rizvi, Director of the Sindh Institute of Urology and Transplantation, described her during a memorial in her honor.
Pfau’s approach to her work stemmed from this premise: She believed compassion and service to the ailing was fundamental to the healing process. She considered the psychology of a disease the most important starting point of its treatment. Nothing is more debilitating than for ailing people to be humiliated and shamed. But in Pakistan, before Pfau came along, leprosy was so stigmatized, patients could not take a doctor’s sympathy or even understanding for granted.
Pfau’s holistic approach was antithetical to modern medicine, in its context of specialization and curative treatment in an exclusively hospital-based environment. Pfau’s was a proactive and pre-emptive approach aimed at preventing the disease, rather than waiting for patients to come in and be treated after they had fallen ill.
For Pfau, treating leprosy did not just mean curing a disease with specific medical conditions affecting the skin. It meant addressing a community and the families in its folds. It also meant rehabilitating the patient. This is essential, as leprosy and similar diseases are caused by conditions spawned by poverty, namely poor sanitation, malnutrition and crowding. Poverty is created by a society that rejects the concept of egalitarianism and an equitable distribution of wealth.
Poverty can be defeated by an educated, conscientious and self-aware citizenry. This alone could drive away ignorance, one major enemy of good health. Information and knowledge are key factors in the prevention of diseases such as leprosy. Pfau realized this right away, and she adopted a strategy of countering the prevailing ignorance by disseminating knowledge about leprosy through talks, lectures and workshops in communal environments such as schools, clubs and other institutions.
These measures helped lower the prevalence of leprosy and ultimately turned it into a manageable disease. The curative measures, which Pfau implemented next, were essential to nearly wiping out all traces of the scourge in Pakistan.
Her initial holistic approach on its own made a big impact on leprosy in Pakistan. The number of cases went down remarkably, but she knew total control was not possible if her team sat back and relaxed. Even today, new cases crop up and the disease resurges, which is why it is essential to monitor communities and begin treatment as soon as symptoms appear. To nip the disease in the bud, it is important not just to save the individual patient, but also to prevent new cases. Because the incubation period of leprosy can be as long as 20 years, monitoring recurrences can be a tedious process, but it has to be done. In fact, this lengthy monitoring period can promote bonding between leprosy patients, their families and health workers. Such is the case at the Marie Adelaide Leprosy Centre (MALC) in Karachi, which Pfau helped develop. MALC now serves as a hub for the 157 leprosy treatment centers dispersed throughout the country.
Pfau’s most important contribution to medical science was her practice of holistic healing. She considered it important to restore the dignity of leprosy patients by reintegrating them in society while also curing their bodies. To this end, she traveled all over Pakistan to visit patients and their families, mingle with them, hug them, dine with them—and she taught her team to do the same. She was shocked by families’ rejection of their own kin who suffered from leprosy. Her way of neutralizing this attitude was to step forward herself, teaching by demonstration and extending acceptance to the victims of society’s prejudices.
Will Pfau’s legacy continue? It should, because she trained a strong team, boosting its members’ confidence by acknowledging their contributions to leprosy health care. Hopefully, her approach to medicine will spread to other countries as well. They need it.
Your support matters…Independent journalism is under threat and overshadowed by heavily funded mainstream media.
You can help level the playing field. Become a member.
Your tax-deductible contribution keeps us digging beneath the headlines to give you thought-provoking, investigative reporting and analysis that unearths what's really happening- without compromise.
Give today to support our courageous, independent journalists.






You need to be a supporter to comment.
There are currently no responses to this article.
Be the first to respond.